Effective pain management in the prehospital and emergency environment is a craft as long as an expertise. PUAEME008 Provide Pain Monitoring brings structure to that craft. The device concentrates on evaluation, intervention, and continual review, and it sits at the junction of clinical judgment, communication, pharmacology, and security. I have actually educated and evaluated countless students via this material for many years, from paramedic pupils to knowledgeable registered nurses looking for to expand their extent. The same themes return every time: clarity in assessment, precision in application, respect for danger, and relentless reassessment.
This post unpacks what the PUAEME008 give discomfort administration device anticipates in method, just how an offer discomfort management training course normally runs, and how specialists in different functions can utilize it to sharpen their discomfort monitoring training. Whether you are exploring brief courses in pain management for intense treatment or going for a pain administration accreditation training course that straightens with ambulance market frameworks, you will certainly find functional details here.
The scientific stakes
Untreated or undertreated pain is not only terrible, it has effects. Pain raises thoughtful drive, elevates heart price and high blood pressure, and gas stress and anxiety. In the injury client it can exacerbate blood loss. In older grownups it contributes to delirium. In kids it threatens depend on and makes complex future treatments. On the other hand, badly chosen or too much analgesia can dispirit air flow, unknown developing pathology, or produce hemodynamic instability. PUAEME008 instructs that balance: deal with pain as the 5th important indication while securing airway, breathing, and circulation.
I recall a rural automobile rollover where the first-on -responder was a volunteer with restricted medicinal choices. They had training lined up with PUAEME008. With organized assessment, they utilized non-pharmacological approaches and titrated breathed in methoxyflurane while waiting for an innovative team. The patient got to the ED with controlled discomfort, intact respiratory tract reflexes, and steady vitals. That result mirrors the system's core method: analyze, intervene thoughtfully, testimonial, and intensify when needed.
What PUAEME008 really covers
The system title is candid: Supply Discomfort Management. Under the hood, it clusters into 3 domains.
Assessment precedes. Learners need to take a pain background with accuracy, map top quality and character, and slow to vitals and context. The device expects fluency with pain ranges like numerical score ranges, Wong-Baker for youngsters, and visual analog devices, and the capacity to adapt when a patient can not self-report, as an example making use of FLACC for preverbal kids or behavior pain ranges for the intubated. It additionally needs situational evaluation: system of injury, warnings recommending time-critical pathology, and environmental elements that may influence both pain and the plan.
Intervention extends both non-pharmacological and pharmacological tools. Non-pharmacological techniques are never just cushioning in this system; they matter. Positioning, splinting, ice or warm where suitable, verbal peace of mind, and active diversion have measurable results. Pharmacology after that layers on: breathed in analgesics like methoxyflurane, nitrous oxide/oxygen blends where readily available, oral representatives such as paracetamol and ibuprofen, and parenteral choices like fentanyl, morphine, or ketamine depending upon the expert's scope and regional protocols. The unit does not transform every student right into a sophisticated life support paramedic. It teaches risk-free, evidence-consistent options within scope.
Review is not a token step. The system bakes in review periods and the assumption of result dimension. Did the pain score drop within mins of the intervention? Did respiratory system price or end-tidal carbon dioxide adjustment? Are sedation scores wandering up? If you can not show renovation or you detect very early adverse effects, you need to change the plan quickly.
Who should consider this discomfort administration course
The audience for PUAEME008 is wide, which belongs to its stamina. It is frequently packaged as a give discomfort management program within emergency situation medical feedback programs and vocational credentials that feed right into ambulance support functions. It also shows up suffering administration training for nurses that operate in immediate treatment, event medicine, or country and remote centers. Numerous physio therapists finishing discomfort administration training courses for physio therapists want to connect hands-on treatment and severe analgesia abilities, particularly in sports or job-related setups where first action matters.
If you already hold a discomfort monitoring certification or a broader pain management accreditation that focuses on chronic discomfort, PUAEME008 will feel more tactical. The focus gets on emergency pain monitoring, intense analysis under time pressure, and short half-life drugs that are titratable with a fast onset. For medical professionals who mainly see postoperative or persistent pain, this provides a corresponding ability set.
What a course looks like in practice
A high quality pain management training program that supplies PUAEME008 normally runs as a mixed program. Anticipate pre-reading on analgesic pharmacology and discomfort physiology, followed by an intensive day of case-based situations, ability terminals, and substitute patients. Training courses vary, however the same spinal column shows up repeatedly: high-fidelity rehearsal of analysis, gauged use medicines, and deliberate experiment monitoring and communication.
Training service providers who take it seriously will analyze not simply technological steps, but how you speak with people, interpret discomfort ratings, and validate dosing decisions to a medical lead over the radio. If you are picking amongst discomfort management training courses, ask the amount of circumstances they run per learner, what tracking devices they utilize, and whether they cover pediatric and senior citizen adaptations. Great short training courses hurting management will consist of tough cases: the intoxicated injury patient, the hypotensive abdominal discomfort, or the person with a substantial opioid resistance who needs escalating application and a safety net.
Understanding discomfort past the score
Pain is subjective, personal, and culturally mediated. Two patients with the very same crack can report discomfort scores at opposite ends of the range. That does not make one of them incorrect. Your job is to secure the patient's summary of pain to operate and to objective dangers. Can they take a complete breath? Can they endure very little motion for packaging and move? Is the pain avoiding you from doing necessary procedures?
PUAEME008 encourages structured inquiry. Where is the pain, and does it emit? What makes it even worse or better? What are the associated symptoms? In breast pain, ask about diaphoresis, nausea, lack of breath. In stomach pain, clarify location, start, and includes that separate surgical from clinical causes. In musculoskeletal injury, seek defect and neurovascular compromise. These details educate the analgesic strategy just as long as the number on the discomfort scale.
Non-pharmacological methods worth mastering
When people photo emergency discomfort monitoring, they believe syringes and inhalers. The quieter wins usually come from the essentials. I have seen individuals change from a pain score of eight to 5 in 2 minutes with absolutely nothing more than mindful splinting and repositioning. An arm supported in a sling minimizes grip on injured cells. A fractured tibia in a well-applied vacuum cleaner splint ends up being tolerable enough to allow mild transportation. Ice bag help in intense sprains and contusions by reducing swelling and numbing surface nerves. Heat makes good sense in muscle convulsion, not in fresh trauma.
Communication becomes part of the analgesic plan, not an afterthought. Discuss what will certainly occur, what feelings to anticipate, and what you need from the patient. Teach paced breathing for the next 2 minutes while you prepare drugs. In pediatric cases, engage the caregiver and usage disturbance tools. Even as you treat the pain, you are measuring the reaction minute by minute.
Pharmacology within scope and context
The precise medicine embeded in a PUAEME008 provide discomfort management training course depends on jurisdiction and carrier range. The usual thread is a tipped, titratable approach.
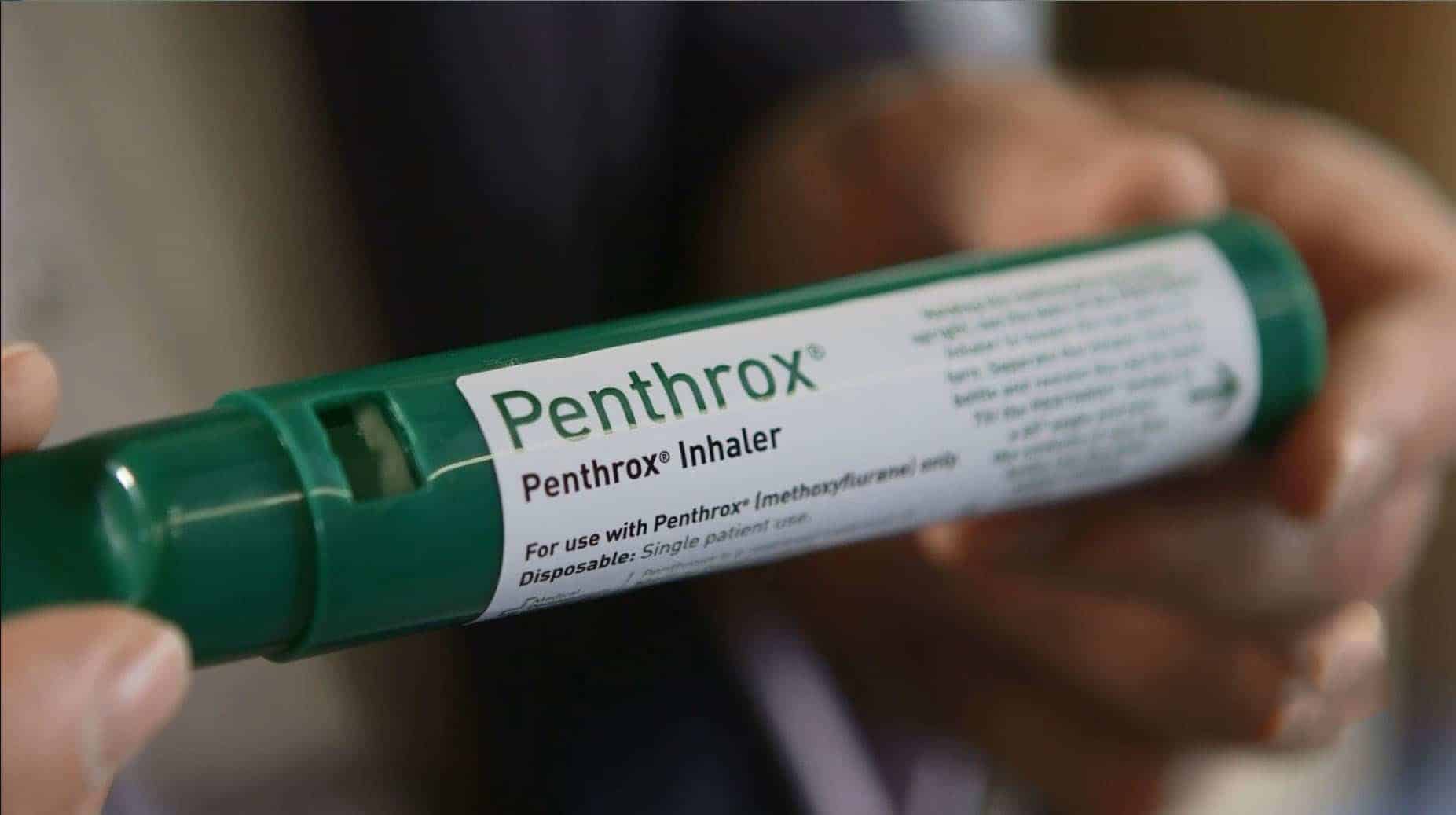
Inhaled alternatives are a Browse this site staple because they have a fast beginning and subside quickly. Methoxyflurane can supply meaningful relief with minimal devices. It requires interest to application restrictions, collective direct exposure, and a dedication to fresh air flow to reduce job-related exposure. Laughing gas 50 percent in oxygen offers trusted analgesia with a benign profile however needs cyndrical tube logistics and checking for nausea, dizziness, or diffusion hypoxia if misused.
Oral agents are occasionally overlooked in immediate care, yet they have value, particularly when the person is steady and transportation times are expanded. Paracetamol and ibuprofen used with each other can create additive impacts. They are not adequate for major trauma, yet they reduce the opioid worry and can reduce rebound pain later.
Parenteral opioid options typically center on fentanyl and morphine. Fentanyl, with its rapid beginning and brief period, can be titrated in tiny increments. It has less histamine launch than morphine, which assists when blood pressure is delicate. Morphine offers deep, longer relief and can be efficient when offered thoroughly with titration and monitoring. Both need careful interest to breathing standing, sedation, and cumulative application. Have naloxone readily available, yet do not depend on it to compensate for bad decision-making.
Ketamine continues to be a beneficial alternative where range allows. In sub-dissociative doses, it provides potent analgesia with marginal respiratory system anxiety. It can elevate blood pressure and heart rate somewhat, which is preferable in particular trauma contexts, and it maintains air passage reflexes. Emergence phenomena at reduced doses are unusual, yet still need preparation and tranquil coaching. Integrating low-dose ketamine with low-dose opioid can produce synergistic relief while lessening the negative account of either medicine alone.
Antiemetics and accessories matter. If the client is wriggling and vomiting, your strategy is not functioning. Ondansetron or similar agents maintain the experience. Small information like having suction all set for a patient that comes to be drowsy can be the distinction between smooth care and a close to miss.
emergency pain managementMonitoring and safety and security nets
Every medication choice sits inside a safety and security framework. Before you begin, you verify the basics: license airway, effective breathing, appropriate circulation. Throughout analgesia, you watch breathing price, oxygen saturation, and where available, end-tidal CO2. You note blood pressure and degree of consciousness. Sedation scales provide you a language to define what you see, instead of unclear words like drowsy or sleepy.
Good method suggests examining result at certain time factors. With inhaled analgesics, you must see purposeful modification within a few breaths and a constant degree within minutes. With IV opioids, initially examine at two to three minutes and once more at 5 to 10 mins prior to repeating doses. Titration maintains you inside a healing home window and constructs trust fund with the client. Paper the baseline rating, the intervention, the moment, and the new rating. This is not paperwork for its very own purpose. It is exactly how you find out what works and area early caution signs.

Special populations and side cases
Pain does absent nicely, and PUAEME008 expects you to adapt.
Children call for dosage adjustments, careful language, and devices like the Wong-Baker faces range. Splinting and adult participation can decrease distress significantly. Some inhaled agents may remain off-label for extremely children, so your course must clarify local policy.
Older grownups procedure medicines in a different way. Minimized kidney feature, polypharmacy, and frailty enhance the threats of sedatives and opioids. Beginning low, go slow-moving, and prioritize non-pharmacological approaches and regional stablizing. A hip fracture patient commonly benefits from well-padded positioning and mild grip, then little aliquots of opioid or low-dose ketamine, always with oxygen and monitoring.
Pregnancy modifications whatever from breathing get to hemodynamics. Placing to prevent aortocaval compression, cautious oxygenation, and consultation with clinical control take concern. Certain drugs might be contraindicated depending on pregnancy. The device's standards will accept local procedures and assessment pathways.
Intoxicated or head-injured patients position a tracking obstacle. You can not rely upon behavior alone to judge sedation. In such instances, maintain dosages little, reconsider students and ventilation typically, and keep a reduced threshold for innovative air passage support if awareness drifts. Discomfort still requires therapy, but the margin for error narrows.
Opioid-tolerant clients will certainly not react to common dosages. It is simple to undertreat them out of concern, after that view them relocate uncontrollably on a spine board. Titrate assertively while keeping oxygen and respiratory tract equipment ready. Low-dose ketamine can be vital right here. File their baseline opioid usage; it validates your dosing and guides handover.
Communication and handover
Clear, concise communication multiplies the worth of great professional job. When you hand over an emergency pain administration patient, provide a timeline. As an example, you may claim that the person's left wrist deformity was splinted at 14:20, methoxyflurane began at 14:22, discomfort rating fell from eight to five by 14:25, and 50 micrograms of fentanyl IV were titrated in between 14:28 and 14:35 with a present discomfort rating of three. Include vitals, sedation degree, and any kind of negative events. This story lets the receiving clinician make logical next actions instead of beginning with zero.
Most discomfort administration training programs will certainly drill this kind of handover. It may really feel repeated in the classroom, yet it pays off when your client rolls into a jampacked ED where attention is scarce.
Risk management and legal considerations
Analgesia is not exercised in a vacuum. You function within business policies, medicine authorizations, and an advancing proof base. PUAEME008 advises you to confirm your scope, follow local professional practice standards, and consult when offered with complicated or contraindicated situations. Documentation is not simply security, it is continuity of care. If you believe a medication is suggested but the circumstance differs common methods, rise to a clinical lead, record the examination, and relocate carefully.
Environmental dangers matter too. Making use of methoxyflurane in a badly ventilated area boosts occupational exposure. Providing nitrous oxide without scavenging can leave the staff lightheaded. Climate, darkness, and terrain can transform easy tasks right into hazards. An excellent provide pain administration training course will tip outside the classroom and reveal you how to administer analgesia in a cramped shower room, on a football field, or next to a roadway with web traffic inches away.
How to choose a quality provider
Not all discomfort administration courses are developed equal. Seek trainers with frontline experience, not just showing qualifications. Ask whether the training course consists of pediatric and geriatric cases, air passage tracking abilities, and unfavorable occasion management. Simulation ought to worry decision-making, not simply technological steps. The best discomfort administration training programs supply post-course assistance, such as quick-reference application overviews and access to refresher scenarios.
If you are a nurse seeking pain administration training for registered nurses, choose a supplier who comprehends nursing range and typical job settings. For physiotherapists, discover pain monitoring programs for physio therapists that incorporate movement-based approaches and splinting with analgesia concepts. Those pursuing a pain management certification or discomfort management certification ought to make sure the content maps to acknowledged frameworks and consists of reputable analysis, not just attendance.
The useful circulation at scene
Below is a small field-tested flow you can adapt. Maintain it sincere and adaptable, not rote.
- Scene safety and security, main study, and prompt life dangers managed. While you handle air passage and blood loss, ask a solitary pain inquiry to set the stage. Focused discomfort evaluation: area, quality, intensity, useful limitations, warnings. Pick an appropriate pain scale. Non-pharmacological actions: placement, splint, ice or heat, calm training. Begin these before meds. Pharmacological plan within extent: select the simplest effective representative, titrate slowly, monitor very closely with recorded time points. Review at specified periods. If the discomfort rating does not drop or damaging impacts appear, adjust the strategy or rise for sophisticated support.
Building sturdy competence
Competence does not come from a certification alone. It originates from reps, reflection, and feedback. After a tough situation, assess it. Did you choose the best representative? Was your very first dosage as well timid or too bold? Did you reassess at the correct times? Talk with colleagues and instructors. The unit PUAEME008 provide discomfort administration anticipates reflective technique. When you come across an uncommon negative result or a persistent pain disorder that resists your first-line choices, create it up and share the lessons with your team.
Consider routine refreshers. Skills like formulating little fentanyl aliquots under tension, mentoring a frightened kid through inhaled analgesia, or stabilizing ketamine's benefits versus periodic dysphoria get corroded without technique. Short training courses hurting monitoring make sense as annual or biennial updates, specifically if your office modifications procedures or adds new agents.
From certificate to capability
A discomfort management certificate or pain management accreditation looks clean theoretically. What matters is just how your clients experience your care. They do not bear in mind the system code. They bear in mind the paramedic who splinted their leg gently, described the strategy, timed each dosage with their breathing, and stayed present until the pain relieved. They keep in mind the nurse who located a comfortable position for a fractured neck of femur and made use of little, regular doses to make movement acceptable. They remember dignity restored.
If you are evaluating whether to sign up in a discomfort administration certificate training course, ask on your own what you want from it. If it is a badge, you will obtain one. If it is capacity, look for a provide pain monitoring program that makes you practice real-life intricacy, tracks your choices, and gives frank responses. The right program constructs your judgment, not simply your medication list.
Final thoughts for the field
Pain monitoring is a moral commitment and a medical ability. PUAEME008 offers a practical framework that stands up in the unforeseeable world of prehospital and immediate care. Utilize it to sharpen your evaluation, broaden your treatments, and tighten your review loopholes. Respect the pharmacology, maintain your surveillance truthful, and treat each client's pain as genuine, also when it provides differently than you expect.
The finest medical professionals treat the individual in front of them, not a method laminated on a clipboard. They recognize the regulations well enough to follow them and, when required, to safely request assistance when the guidelines do not quite fit. That is the standard worth aiming for when you lay out to provide pain monitoring in the minutes that matter.